You noticed your leg is swollen. Maybe it started after surgery, maybe after cancer treatment. Or maybe it appeared slowly, with no clear reason at all. You pushed on the skin, and it left a dent. Your ankle won’t fit into your shoe.
Now you’re searching for answers, and probably scared.
You’ve heard the word lymphedema from a doctor. But no one has sat down and told you what it actually means, what’s happening inside your body, or what comes next.
This guide will change that. By the end, you’ll understand exactly what lymphedema is, why it happens, what stage you may be at, and, most importantly, what you can do about it.
If you’re newly diagnosed, early action genuinely changes your long-term outcome. This is one of those conditions where waiting costs you.
| Ready to speak with a specialist? Dr Jeremy Sun is Singapore’s leading lymphedema microsurgery specialist. If you’ve just been diagnosed or suspect you have lymphedema, early consultation gives you the widest range of treatment options. Book a consultation at LymphEdAsia → lymphedasia.com |
What Exactly Is Lymphedema, and What’s Happening Inside Your Body?
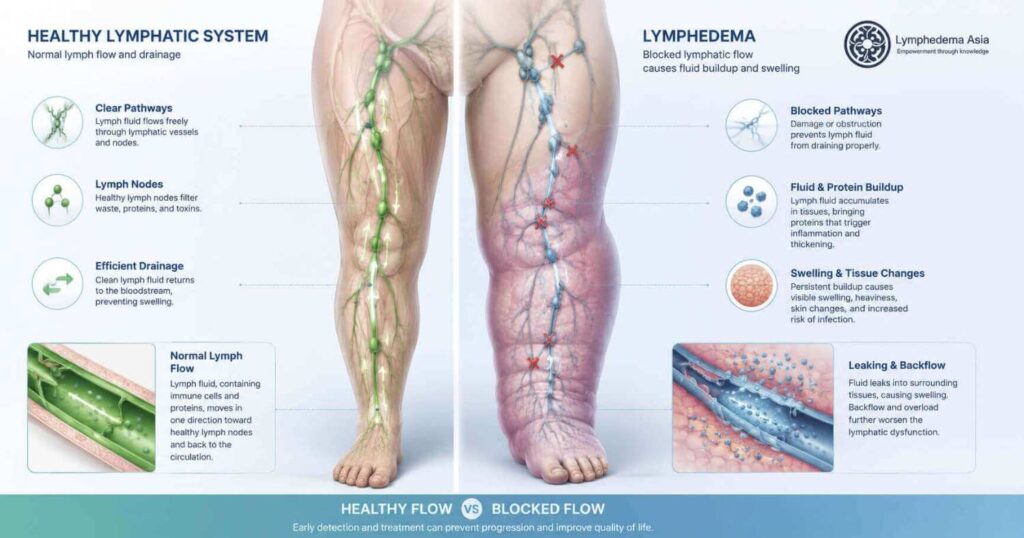
Lymphedema (also spelt lymphoedema) is a chronic condition where lymph fluid builds up in your body’s soft tissues, most often in an arm or leg, and causes persistent, painful swelling.
To understand why this happens, you need to know a little about your lymphatic system. Think of it as your body’s drainage network. It runs parallel to your blood vessels and carries a clear fluid, lymph fluid, away from your tissues and back into your bloodstream.
This fluid contains proteins, waste products, and immune cells. Under normal conditions, lymph nodes filter this fluid and pass it along through a series of vessels. Your body produces around 2–3 litres of lymph fluid every day.
When part of this network is damaged or missing, through surgery, radiation, infection, or a structural problem present from birth, the fluid has nowhere to drain. It accumulates. The tissue swells. And over time, the protein-rich fluid triggers inflammation that progressively thickens the tissue.
This is what separates lymphedema from ordinary swelling after an injury. Ordinary swelling resolves on its own in days or weeks. Lymphedema does not resolve on its own. It is a long-term condition that requires active management.
In clinical practice, this means: the longer lymphedema goes unmanaged, the harder it becomes to treat. The fluid that sits in your tissue eventually causes structural changes, fibrosis, that cannot be reversed.
What Causes Lymphedema? Why Did This Happen to You?
Lymphedema falls into two broad categories based on its cause. Understanding which type you have shapes every treatment decision going forward.
Primary Lymphedema: When Your Lymphatic System Didn’t Develop Properly
Primary lymphedema is caused by an abnormality in the lymphatic system that you were born with, even if the swelling only appears later in life. It can show up in infancy (Milroy disease), around puberty (lymphedema praecox), or after age 35 (lymphedema tarda).
It affects women more than men and most often appears in the legs. It’s less common than secondary lymphedema, but it’s frequently missed or misdiagnosed for years.
Secondary Lymphedema: When Something Damages Your Lymphatic System
Secondary lymphedema is the most common type worldwide, and it develops when your lymphatic system is damaged by an external cause. The most common triggers include:
- Cancer treatment: Surgery that removes lymph nodes (such as axillary node dissection for breast cancer) or radiation that scars lymphatic vessels is the leading cause of lymphedema in high-income countries.
- Infection: In tropical regions, a parasitic infection called filariasis, spread by mosquitoes, is the most common global cause of lymphedema, affecting an estimated 120 million people worldwide, according to the World Health Organisation.
- Trauma or surgery: Any procedure that disrupts lymph nodes or vessels in a limb can trigger lymphedema, including vascular surgery, joint replacement, or significant soft tissue injury.
- Obesity: Excess body weight places sustained pressure on lymphatic vessels, reducing their drainage capacity over time.
- Chronic venous insufficiency: When veins can’t return blood efficiently, it overwhelms the lymphatic system’s capacity to compensate.
| DR. SUN’S CLINICAL PERSPECTIVE“In my practice, I see patients who have lived with swelling for years before they receive a correct diagnosis. The most common scenario is a woman treated for breast cancer five, seven, or even ten years earlier, who gradually noticed her arm feeling heavier, but never connected it to her surgery. By the time they reach me, many have significant fibrotic changes in the tissue that would have been entirely preventable with early intervention. This means for patients: if you have any risk factors for lymphedema, particularly a history of cancer treatment involving lymph node removal or radiation, do not wait for the swelling to become obvious before seeking specialist review. Dr Jeremy Sun | Lymphedema Microsurgery Specialist, Singapore |
How Do You Know If Your Swelling Is Lymphedema?
Lymphedema has a distinctive pattern of symptoms that sets it apart from other causes of swelling. You may not have all of these, but recognising the cluster is important.
Common Signs to Look For
- Persistent swelling in an arm, leg, hand, or foot that doesn’t resolve with elevation or rest overnight
- A feeling of heaviness, tightness, or fullness in the affected limb, often before visible swelling appears
- Reduced range of motion or difficulty bending a joint in the affected area
- Aching, discomfort, or recurring infections (cellulitis) in the swollen area
- Skin changes over time: thickening, hardening, or a texture change that clinicians call peau d’orange (skin resembling orange peel)
- Jewellery, clothing, or shoes that suddenly feel too tight on one side of your body
- Pitting: when you press the skin firmly, and it leaves an indentation that takes more than a few seconds to return, though note that in later stages, fibrosis means the skin may no longer pit
What lymphedema is not: Bilateral leg swelling (both legs equally) is more commonly caused by heart, kidney, or liver conditions, or medication side effects. Sudden, severe swelling following injury is also different. A lymphedema specialist can distinguish these clearly.
What Stage Is Your Lymphedema At? Understanding the ISL Scale
Lymphedema is classified into stages by the International Society of Lymphology (ISL). Knowing your stage helps you and your specialist choose the right treatment approach.
| Stage | What It Means | What You’ll Notice | Reversible? |
|---|---|---|---|
| Stage 0 (Subclinical) | Lymphatic damage exists, but no visible swelling yet | The limb may feel heavy or different. No obvious swelling. Detectable only by specialist assessment. | Yes, ideal stage to intervene |
| Stage 1 (Mild) | Visible swelling that reduces when you elevate your limb overnight | Pitting oedema. The limb feels full. Returns to near-normal size with rest. | Mostly, the best window for conservative treatment |
| Stage 2 (Moderate) | Swelling no longer reduces with elevation. Tissue begins to harden. | Constant swelling, skin tightening, and reduced limb function. Increased infection risk. | Partially requires active management |
| Stage 3 (Severe / Elephantiasis) | Irreversible fibrosis. Extreme swelling. Major skin changes. | Very large limb, skin hardening, recurring infections, significant disability. | No, but surgical options can reduce volume. |
In clinical practice, this means: most patients who reach Dr Sun’s clinic are at Stage 1 or Stage 2, and many still have excellent treatment options available. The goal is to prevent progression to Stage 3, where surgical intervention becomes the primary tool.
How Is Lymphedema Diagnosed? What Tests Will You Need?
A diagnosis of lymphedema is primarily clinical, meaning it’s based on your medical history, your symptoms, and a physical examination. No single blood test confirms it. But several investigations help confirm the diagnosis and guide treatment.
Investigations Your Specialist May Request
- Limb volume measurement: Using water displacement or sequential circumference measurements, your specialist establishes a baseline and tracks changes over time.
- Lymphoscintigraphy (nuclear medicine scan): A small amount of radioactive tracer is injected into the hand or foot and imaged as it travels through your lymphatic vessels. This is the gold-standard imaging test for confirming lymphedema and mapping your lymphatic network.
- ICG lymphography (indocyanine green): A newer technique where a fluorescent dye is injected and tracked using near-infrared imaging. It gives real-time visualisation of lymphatic flow and is used extensively in surgical planning.
- MRI or ultrasound: Sometimes used to exclude other causes of swelling and to assess tissue changes.
Your GP can refer you directly to a lymphedema specialist for assessment. You do not need to wait until your swelling is severe to seek evaluation; in fact, the earlier the better.
What Are Your Treatment Options? From Compression to Surgery
There is no cure for lymphedema, but it can be very effectively controlled, and in many cases, significantly improved. Treatment exists on a spectrum, from conservative daily management through to advanced microsurgical procedures.
Conservative Management: The Foundation of Lymphedema Care
Complete Decongestive Therapy (CDT) is the internationally accepted first-line treatment for lymphedema. It has two phases: an intensive treatment phase and a long-term self-management phase.
CDT combines four components:
- Manual Lymphatic Drainage (MLD): A specialised massage technique performed by a trained therapist that redirects lymph fluid toward functioning lymphatic pathways.
- Compression bandaging and garments: Medical-grade compression wrapping or garments that prevent fluid from re-accumulating.
- Therapeutic exercise: Specific movement patterns that use muscle contractions to push lymph fluid through your system.
- Skin care: Protecting the skin from infection and dryness reduces the risk of cellulitis, a common and dangerous complication.
CDT is effective for Stages 1 and 2 lymphedema and remains essential even for patients who undergo surgery.
Surgical Options: When Is Surgery Appropriate?
Surgical treatment for lymphedema has advanced significantly over the past decade. Two microsurgical procedures now offer a genuine long-term reduction in lymphedema burden.
- Lymphaticovenous Anastomosis (LVA): Tiny lymphatic vessels are connected directly to nearby veins under high-powered microscopy. This creates a new drainage route that bypasses the damaged lymphatic network. LVA is most effective at Stages 1–2 before significant fibrosis has developed.
- Vascularised Lymph Node Transfer (VLNT): Healthy lymph nodes are transplanted from a donor site (such as the groin or neck) to the affected area. This can help regenerate lymphatic function and has shown durable results in Stage 2–3 patients.
- Liposuction (suction-assisted protein lipectomy): For Stage 3 patients with significant fat deposition from chronic lymphedema, specialised liposuction removes the solid protein deposits. This does not treat the underlying lymphatic problem and must be combined with lifelong compression.
In clinical practice, this means: the right surgical option depends entirely on your stage, the anatomy of your lymphatic system, your overall health, and your treatment goals. A specialist assessment, including ICG lymphography, is needed before any surgical recommendation can be made. Surgery is not appropriate for everyone, but for carefully selected patients, it can be life-changing.
| Are you a candidate for lymphedema microsurgery? Dr Jeremy Sun specialises in LVA and VLNT procedures and has treated patients from across Asia and beyond. He offers detailed lymphatic mapping and personalised surgical planning for appropriate candidates. Request a consultation at lymphedasia.com → |
Can You Live a Full Life with Lymphedema? What Long-Term Management Looks Like
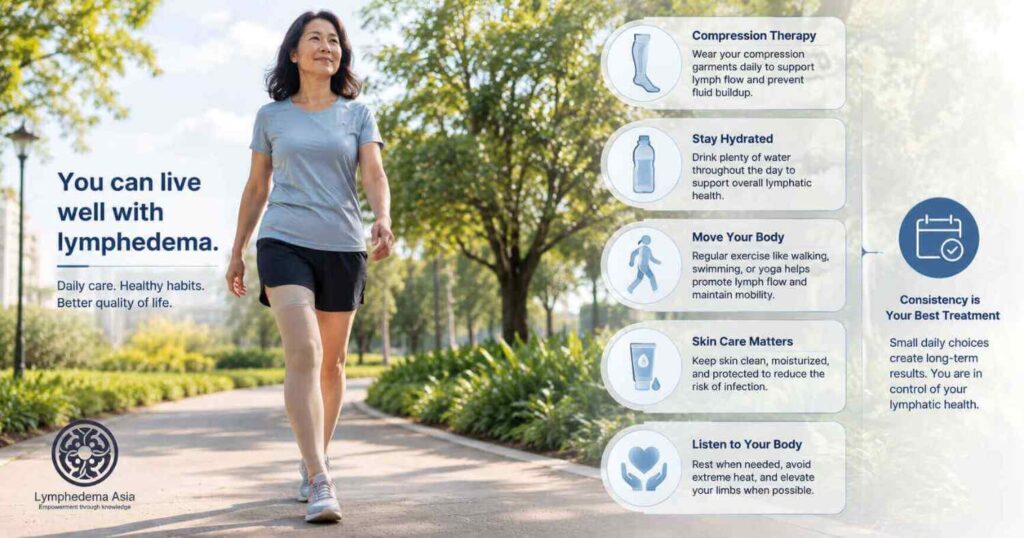
Yes, with the right management, most people with lymphedema live active, full lives. But lymphedema is not a condition you manage for six months and then forget. It requires ongoing attention.
What long-term management typically involves:
- Wearing compression garments daily: medical-grade sleeves or stockings that prevent fluid from re-accumulating
- Regular exercise: including swimming, walking, and targeted limb exercises
- Careful skin care: moisturising daily, protecting against cuts and infection, watching for early signs of cellulitis
- Avoiding extreme heat: including saunas, hot tubs, and prolonged sun exposure, which dilates blood vessels and worsens fluid accumulation
- Travel precautions: wearing compression during flights and long-haul travel, staying hydrated
- Weight management: excess body weight makes lymphedema significantly harder to control
- Regular specialist review, especially if your symptoms change, worsen, or if you develop infections
Lymphedema does not have to define or limit your life. Many patients, including those who have undergone treatment with Dr Sun, return to sport, travel, work, and daily activities with well-controlled lymphedema.
Is It Time to See a Lymphedema Specialist? Three Signs You Shouldn’t Wait
Many people delay seeking specialist care because their swelling doesn’t seem “bad enough.” This is one of the most common and most costly mistakes in lymphedema management.
You should seek specialist review if:
- Your swelling has persisted for more than a few weeks and doesn’t fully resolve overnight with your leg or arm elevated
- You have had cancer treatment, especially involving lymph node removal or radiation, and you notice any new heaviness, tightness, or size difference in a limb
- You are experiencing recurring skin infections (cellulitis) in the same area — this is a sign that your lymphatic system is compromised and under stress.
| Take Action Before Lymphedema Progresses. Understanding what lymphedema is is the first step. The second is speaking with someone who can assess your specific situation and give you a clear path forward. Dr Jeremy Sun consults at LymphEdAsia in Singapore and sees patients from across Southeast Asia, Australia, and internationally. His clinic offers complete lymphatic assessment, including ICG lymphography and microsurgical evaluation, in a single specialist setting. Early treatment means more options, better outcomes, and a smaller impact on your daily life. The best time to seek help is now. Book your consultation at lymphedasia.com → |
| Key Takeaways: Lymphedema is a chronic condition caused by damage to or abnormality of the lymphatic system, resulting in persistent fluid buildup, most commonly in an arm or leg. It does not resolve on its own. Early diagnosis and treatment prevent progression to irreversible stages. Treatment options range from conservative management (CDT, compression) to advanced microsurgery (LVA, VLNT); the right approach depends on your stage and anatomy. Long-term management is a daily commitment, but with the right support, most people with lymphedema live full and active lives. If you have risk factors or symptoms, don’t wait for the swelling to become severe. Early specialist review opens more treatment doors. |