Welcome to an in-depth exploration of cellulitis and lymphoedema, two distinct yet interconnected conditions that can significantly impact quality of life. This guide offers a comprehensive overview, covering risk factors, treatment options, and the crucial role of early detection and management. Whether you’re a patient, caregiver, or healthcare professional, understanding these conditions is the first step toward effective care.
Understanding Cellulitis
What is Cellulitis?
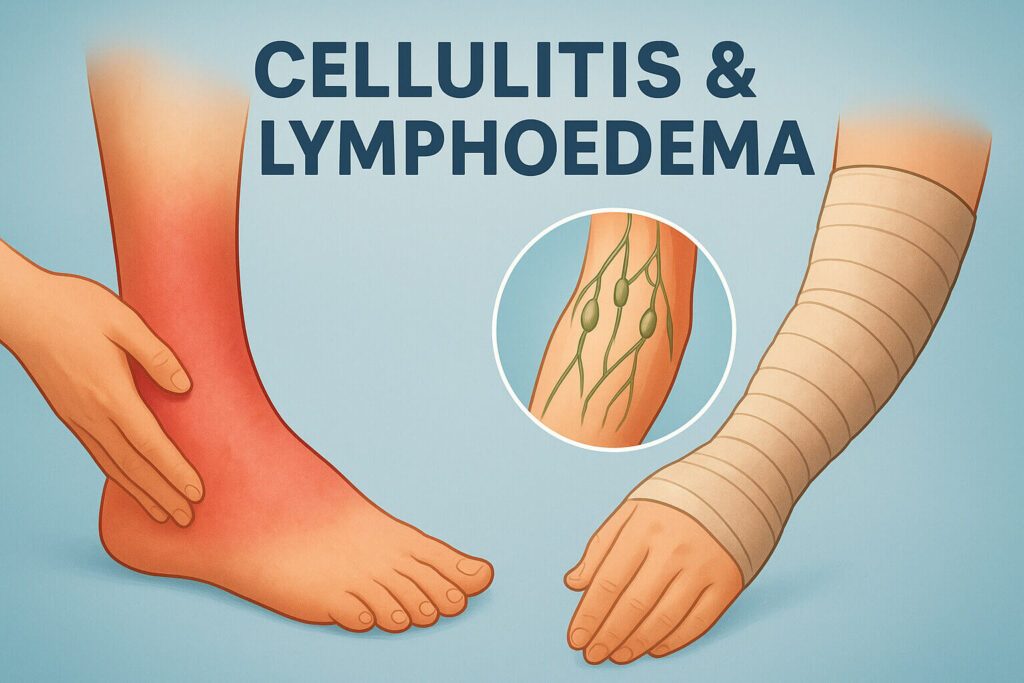
Cellulitis is a common, potentially serious bacterial skin infection. Streptococcus and staphylococcus are usually the culprits, entering through a break in the skin. Prompt treatment with an antibiotic is crucial to prevent complications. It is essential to recognize the signs of infection early to avoid more serious health issues related to cellulitis. [Insert Internal Link]
Common Cellulitis Symptoms
Signs of cellulitis typically include redness, swelling, and pain in the affected area. Fever may also be present, indicating a systemic response to the skin infection. Other signs of cellulitis may include warmth to the touch, tenderness, and sometimes blisters. Early recognition of these symptoms is crucial for effective treatment of cellulitis.
Cellulitis Risk Factors for Patients
Several factors increase the risk of developing cellulitis. A break in the skin, such as a cut, insect bite, or surgical wound, provides an entry point for bacteria. Patients with lymphoedema are at a higher risk of cellulitis due to impaired lymphatic drainage. Other risk factors for cellulitis include obesity, diabetes, and a history of recurrent cellulitis. [Insert Internal Link]
Exploring Lymphoedema
What is Lymphoedema?
Lymphoedema is a chronic condition characterized by swelling, most commonly in a limb, caused by a buildup of lymph fluid. This occurs when the lymphatic system, responsible for draining fluid, is impaired or damaged. Effective management involves compression bandages and specialized skin care. Lymphoedema can significantly affect a person’s quality of life.
Primary vs. Secondary Lymphedema
Lymphoedema is classified as either primary or secondary lymphedema. Primary lymphedema is rare and results from genetic mutations affecting lymphatic system development. Secondary lymphedema is more common and arises from damage to the lymphatic system, often due to cancer or its treatment, including lymph node removal. Distinguishing between primary and secondary lymphedema is crucial for tailored management.
Lymphoedema of the Arm: Causes and Symptoms
Lymphoedema of the arm, or arm lymphoedema, frequently develops as a result of breast cancer treatment, especially after lymph node dissection or radiation therapy. The causes of lymphoedema of the arm disrupt normal lymphatic drainage, leading to swelling. Key symptoms include a heavy feeling in the affected limb, tightness, and decreased range of motion. Early diagnosis and treatment are important.
The Connection Between Cellulitis and Lymphoedema
How Cellulitis Affects Lymphoedema
Cellulitis significantly impacts those with existing lymphoedema. The impaired lymphatic system, already compromised in its ability to drain lymph fluid, becomes even more vulnerable when a skin infection like cellulitis takes hold. This can exacerbate the lymphoedema, leading to increased swelling, pain, and a higher risk of developing further complications. Prompt treatment of cellulitis is crucial for these patients.
Factors Associated with Cellulitis in Lymphoedema
Several factors contribute to the heightened risk of cellulitis in lymphoedema. A break in the skin, often unnoticed, provides an easy entry point for bacteria like streptococcus and staphylococcus. Reduced immune function in the affected limb due to impaired lymphatic drainage further increases the risk of cellulitis. Additionally, chronic inflammation associated with lymphoedema can compromise the skin’s integrity, making it more susceptible to skin infection.
Managing the Risk of Infection
Managing the risk of infection, especially cellulitis, in patients with lymphoedema requires a multifaceted approach. Meticulous skin care is paramount; this includes daily moisturizing to prevent cracks in the skin. Prompt attention to any breaks in the skin, no matter how small, with thorough cleaning and application of an appropriate ointment is essential. Compression bandages help manage swelling and improve lymphatic drainage, reducing the risk of cellulitis.
Risk Factors for Developing Lymphoedema
Identifying Key Risk Factors
Identifying key risk factors for developing lymphoedema is crucial for early intervention and prevention. For primary lymphedema, genetic predisposition plays a significant role. However, secondary lymphedema, which is more common, has clearer risk factors such as cancer or its treatment. Lymph node removal or radiation therapy, especially in breast cancer treatment, significantly increases the risk of lymphedema. Awareness is key to managing the risk of lymphedema.
Preventive Measures for Patients with Primary or Secondary Lymphedema
Whether dealing with primary or secondary lymphedema, several preventive measures can help mitigate the risk of developing more severe symptoms. Maintaining a healthy weight reduces strain on the lymphatic system. Regular exercise, particularly exercises designed to promote lymphatic drainage, can improve lymph flow. Proper skin care is vital, including moisturizing to prevent breaks in the skin that could lead to cellulitis. The bandage can also help prevent further issues.
Understanding Swell Patterns in Lymphoedema
Understanding swelling patterns in lymphoedema is essential for effective management and early detection of complications. Swelling typically starts gradually, often in the distal parts of the affected limb, such as the hand or foot. It may fluctuate throughout the day, worsening with activity and improving with rest. A sudden increase in swelling, especially if accompanied by pain, redness, or fever, could indicate the onset of cellulitis requiring treatment.
Treatment Options for Cellulitis
Medical Treatments for Cellulitis
Medical treatments for cellulitis typically involve antibiotics, prescribed to combat the bacterial skin infection caused by streptococcus and staphylococcus. The specific antibiotic and duration of treatment depend on the severity of the cellulitis and the patient’s overall health. It’s essential to complete the full course of antibiotics, even if symptoms improve, to ensure the infection is eradicated and to minimize the risk of developing antibiotic resistance. If cellulitis is left untreated, it can have dangerous consequences and affect the lymph system.
Home Remedies and Lifestyle Changes
In addition to medical treatments, home remedies and lifestyle changes can complement the healing process for cellulitis. Proper skin care is crucial. Keeping the affected area clean and moisturized helps prevent further breaks in the skin. Elevating the affected limb can reduce swelling and discomfort. Maintaining a healthy lifestyle, including a balanced diet and regular exercise, supports the immune system and promotes overall well-being. Although home remedies should not replace prescribed medication, they can significantly improve the patient’s comfort and healing journey.
How to Treat Lymphedema Effectively
Treating lymphedema effectively requires a multifaceted approach, focusing on managing swelling, improving lymphatic drainage, and preventing skin infection. Compression therapy, using bandages or compression garments, is a cornerstone of lymphedema management, helping to reduce swelling and improve lymph flow. Manual lymphatic drainage, a specialized massage technique, can also promote lymphatic drainage. Meticulous skin care, including moisturizing to prevent breaks in the skin, is essential to minimize the risk of cellulitis in lymphoedema patients. In some cases, surgical interventions may be considered. The effective way to treat lymphedema is consistent care.
Conclusion and FAQs
Recap of Key Points
In summary, cellulitis is a bacterial skin infection requiring prompt treatment with antibiotics, while lymphoedema is a chronic condition characterized by swelling due to impaired lymphatic drainage. Patients with lymphoedema face an elevated risk of cellulitis, necessitating meticulous skin care and proactive management. Identifying risk factors for both conditions is crucial for early intervention and prevention. Effective management of lymphoedema involves compression therapy, manual lymphatic drainage, and vigilant skin care. Understanding the link between cellulitis and lymphoedema helps in managing the patients with lymphedema.
Motivational Final Advice
Living with cellulitis and lymphoedema can be challenging, but with knowledge, proactive management, and a positive attitude, individuals can lead fulfilling lives. Embrace self-care practices, prioritize skin health, and seek support from healthcare professionals and support groups. Remember that early detection and consistent management are key to preventing complications and maintaining quality of life. You are not alone, and with the right tools and support, you can thrive despite these conditions. Be aware of the signs of infection that may occur.
Frequently Asked Questions
Q1: What is the primary cause of secondary lymphedema?
A1: Secondary lymphedema primarily results from damage to the lymphatic system, often due to cancer or its treatment, including lymph node removal or radiation therapy. Breast cancer treatment is a common cause of arm lymphoedema.
Q2: How does cellulitis affect patients with lymphedema?
A2: Cellulitis poses a significant risk to patients with lymphedema, as the impaired lymphatic system is more vulnerable to skin infection. Cellulitis can exacerbate lymphedema symptoms and increase the risk of complications. This can increase the swelling of the affected limb.
Q3: What are the key preventive measures for reducing the risk of cellulitis in lymphedema?
A3: Key preventive measures include meticulous skin care to prevent breaks in the skin, prompt attention to any skin injuries, regular moisturizing, and the use of compression bandages or garments to improve lymphatic drainage. The risk of cellulitis can be reduced with the right measures.
Q4: Can primary lymphedema be prevented?
A4: Primary lymphedema, resulting from genetic mutations, cannot be prevented. However, early diagnosis and management can help mitigate symptoms and prevent complications. Regular visits to lymphology specialists can help manage the condition.
Q5: What role does compression therapy play in managing lymphedema?
A5: Compression therapy is a cornerstone of lymphedema management, using bandages or garments to reduce swelling, improve lymphatic drainage, and prevent further complications. Consistent use of compression is essential for long-term management. It is recommended to follow the treatment in the right way.